Clinical Trials Day: How we can leverage RWE for continued improvements to the behavioral health clinical research ecosystem

On Clinical Trials Day, we recognize an important part of the healthcare infrastructure: the studies that rigorously evaluate new treatments to determine which will be effective and safe for improving patient health. Through the conventional process of assessment, the treatments that succeed will go on to regulatory approval and will be marketed to patients and their providers.
I am a psychologist and a clinical trialist by training and have been part of the clinical trials enterprise for over 20 years. As I reflect on this Clinical Trials Day, I want to recognize important limitations that exist in the behavioral health clinical trials life cycle—and importantly, to offer solutions for how we can address these gaps.
Across therapeutic areas, but especially within the domain of behavioral health, there are at least two major problems with the way clinical trials are traditionally designed and conducted:
- Clinical trial populations are not representative of most patients.
- Clinical trials use endpoints to measure outcomes that differ from those used in clinical practice.
Let’s break down the impact of these problems on patient outcomes. When a new treatment does succeed in its trial and goes to market, there’s still a relatively high likelihood it won’t work for those to whom it is prescribed in routine care settings. The table below highlights the disconnect between traditional trial characteristics and what happens in everyday clinical care. Most Phase III trials (those studies that typically form the basis of a regulatory approval) have a long list of exclusion criteria. Excluding participants with certain other psychiatric conditions that may commonly co-occur in the real world often renders a substantial proportion of a patient population ineligible for the study. That means that even when we think a treatment will work based on the results of a clinical trial, it doesn’t always work the same way when they come to market and are given to a broader and more diverse population.
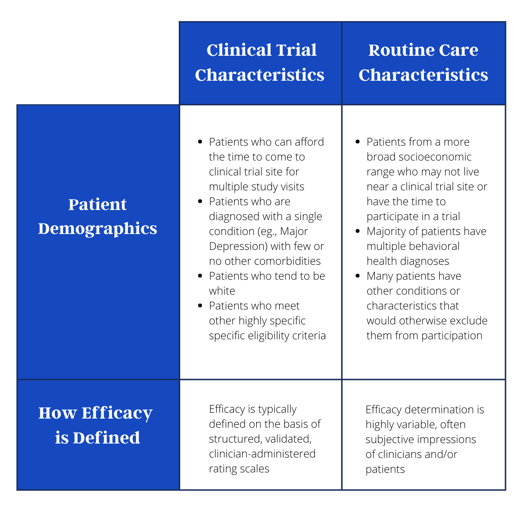
Another challenge of clinical trials is that they often rely on endpoints and outcome measures that are rarely used in real clinical practice (see Table to right). That means we may be testing new treatments against outcomes that do not actually matter to patients or that don’t have an impact on their everyday lives, their symptoms, or their day-to-day functioning.
Both of these are significant gaps—but fortunately, they are gaps that we can start to fill with real-world evidence (RWE), or insights that are generated from real-world data that is captured during routine clinical care via sources such as electronic health records, wearables and other sensors, patient surveys, and insurance claims.
For too long, the research ecosystem has been viewed in black and white; questions are answered either via a clinical trial or via an observational study that generates real-world evidence. In reality, real-world evidence can be used effectively as a complement to traditional clinical trials. Real-world evidence can help to inform the clinical trial process in many ways, including:
- Helping to identify which patients might respond best to a specific treatment–an especially important consideration as the healthcare ecosystem moves toward precision medicine
- Streamlining inclusion and exclusion criteria and determining patient eligibility
- Providing external validity for clinical trial results
- Developing novel endpoints that align more closely with outcomes that matter to patients in the real world
Rigorously conducted randomized clinical trials will always be vital to the healthcare ecosystem and the development of new treatments, and Clinical Trials Day is a great time to recognize their importance. At the same time, we must recognize that new ways to collect a wide range of real-world data present an opportunity to generate new real-world evidence to support the findings resulting from traditional clinical trials. By relying on real-world evidence to inform the decisions we make about treatments, we can ensure that our results are more inclusive–and more likely to help a larger and more diverse group of patients in the real world.


.png)